T cell modifier

CAR2 T-CELL MODIFIER
Thought Experiment on a Novel Receptor for Engineering Cancer-Fighting Cells which is Non-Interfering with the Cancer Fighting Cell
11-May-2023
Bio-Science
Cancer cells are abnormal cells that grow and divide uncontrollably, leading to the formation of tumors or the invasion of nearby tissues. Unlike normal cells, cancer cells do not undergo programmed cell death (apoptosis) when they are damaged or no longer needed by the body. So they need to be killed. Scientists are already making CAR t-cells but they interact with the t-cells. The t-cells are modified but their own receptors are removed. So, when it destroys the cancer cell and the person catches the disease and the immune system hasn’t recovered the receptors it may lead to death. So, in this article we will explore a novel receptor which is not made yet.
Introduction
Acute Lymphoblastic Leukemia (ALL) is a type of cancer that affects the blood and bone marrow, primarily targeting the lymphoid lineage of cells. It is the most common form of leukemia in children but can also occur in adults. ALL is characterized by the rapid production of immature lymphoblasts, or leukemia cells, which accumulate in the bone marrow and interfere with the production of normal blood cells. As a result, new therapies are popping up. Solid cancer can be treated but this is a type of blood cancer so the new therapies. The most well-known therapy is CAR T-cell therapy. But it changes the receptor. So, after the treatment it may take time to recover the receptor and if the person catches the disease that requires the receptor it may lead to death. So in this article we will explore a novel receptor that turns T Cell or Blood Vessel Cell into a cancer fighting cell
Literature Review

Dr. Martin Pule is a renowned physician-scientist known for his contributions to the field of immunotherapy and cellular therapies, particularly in the development of CAR T-cell therapies for cancer treatment. With a background in molecular immunology, he has played a significant role in advancing the design and optimization of CAR T-cell constructs, enhancing their efficacy and safety. Dr. Pule's research focuses on targeting different antigens expressed on cancer cells and optimizing CAR T-cell therapies for hematological malignancies. He has published extensively in prestigious journals, sharing his findings with the scientific community. Additionally, he has been actively involved in clinical trials, evaluating the safety and effectiveness of CAR T-cell therapies and expanding their application to patients who have not responded to conventional treatments. Dr. Martin Pule's work has earned him recognition in the field, and he continues to contribute to the advancement of cellular therapies in oncology.
Hypothesis and Objectives
Binding
The following image (Figure 01) is representing a formal structure of the binding process of a T-Cell and an acute Lymphoblastic Leukemiac Cancer Cell. The Mesothelin receptors bind to Mesothelin. The factors of the T-Cell are initially in-active. The Mesothelin receptors get activated due to close proximity. After that, they activate the inactivate factors.
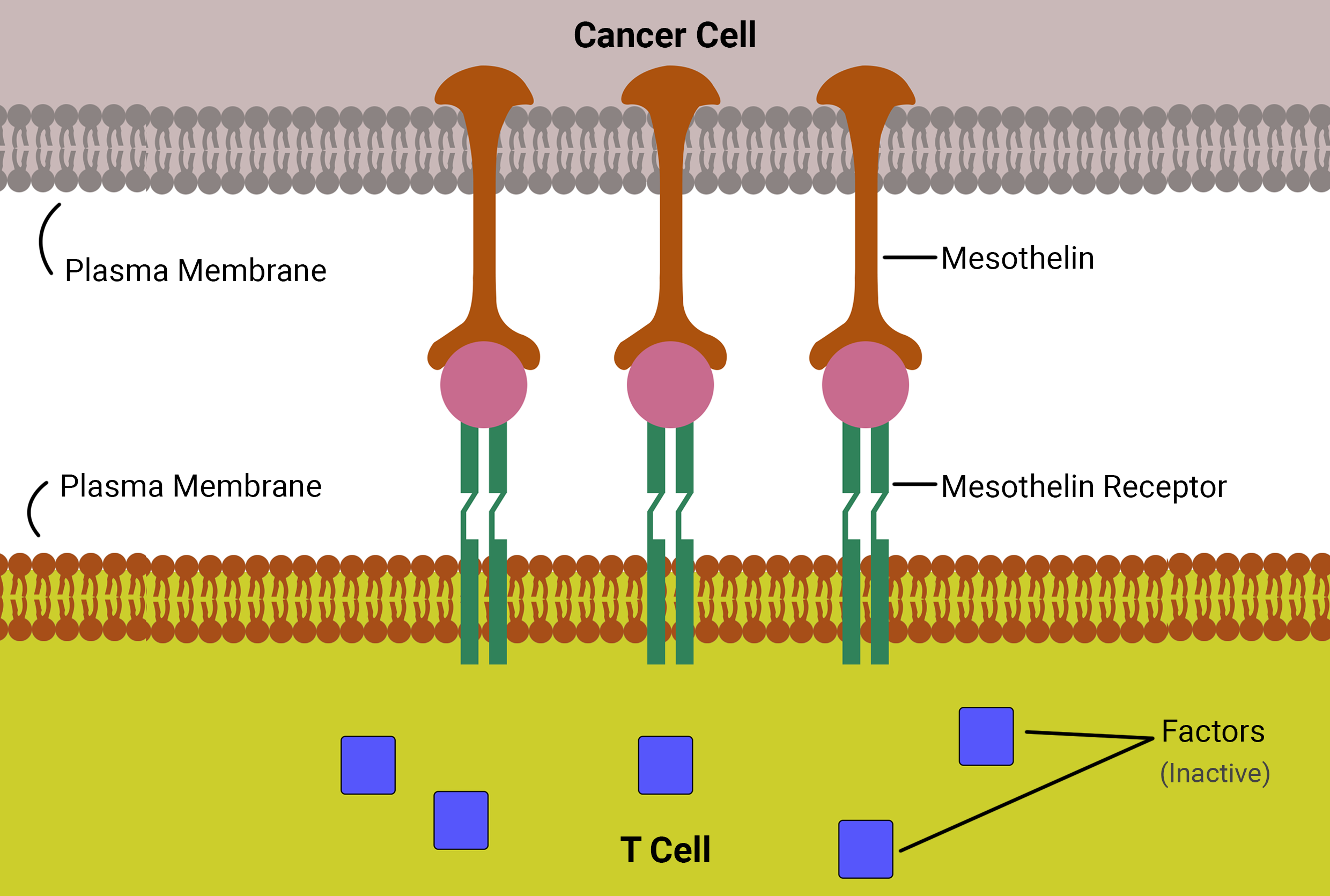
Assembly
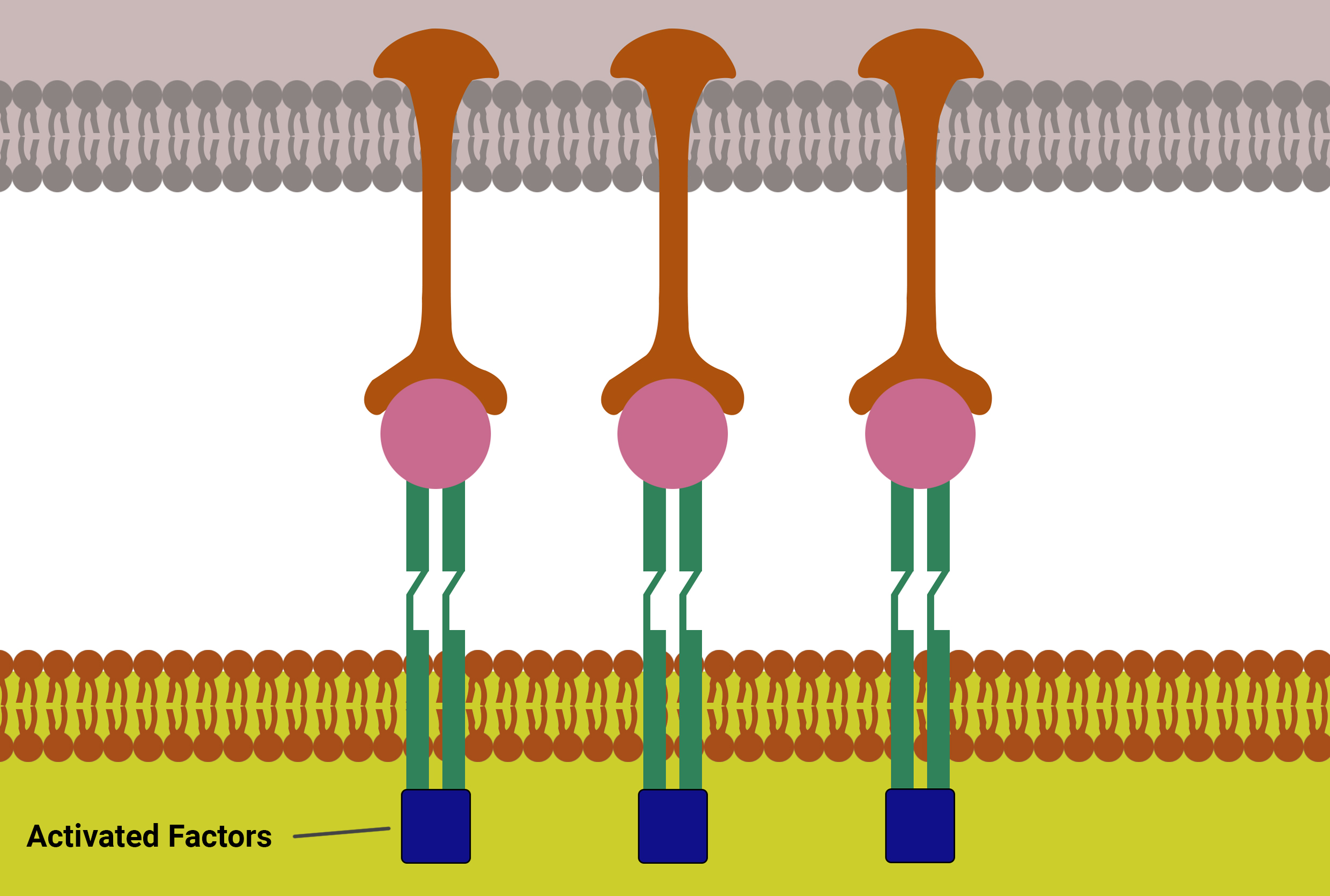
The factors of the T-Cell get connected with the receptors and get activated by conformational change (Figure 02).
After that, the factors disassociate from the receptors (Figure 03).
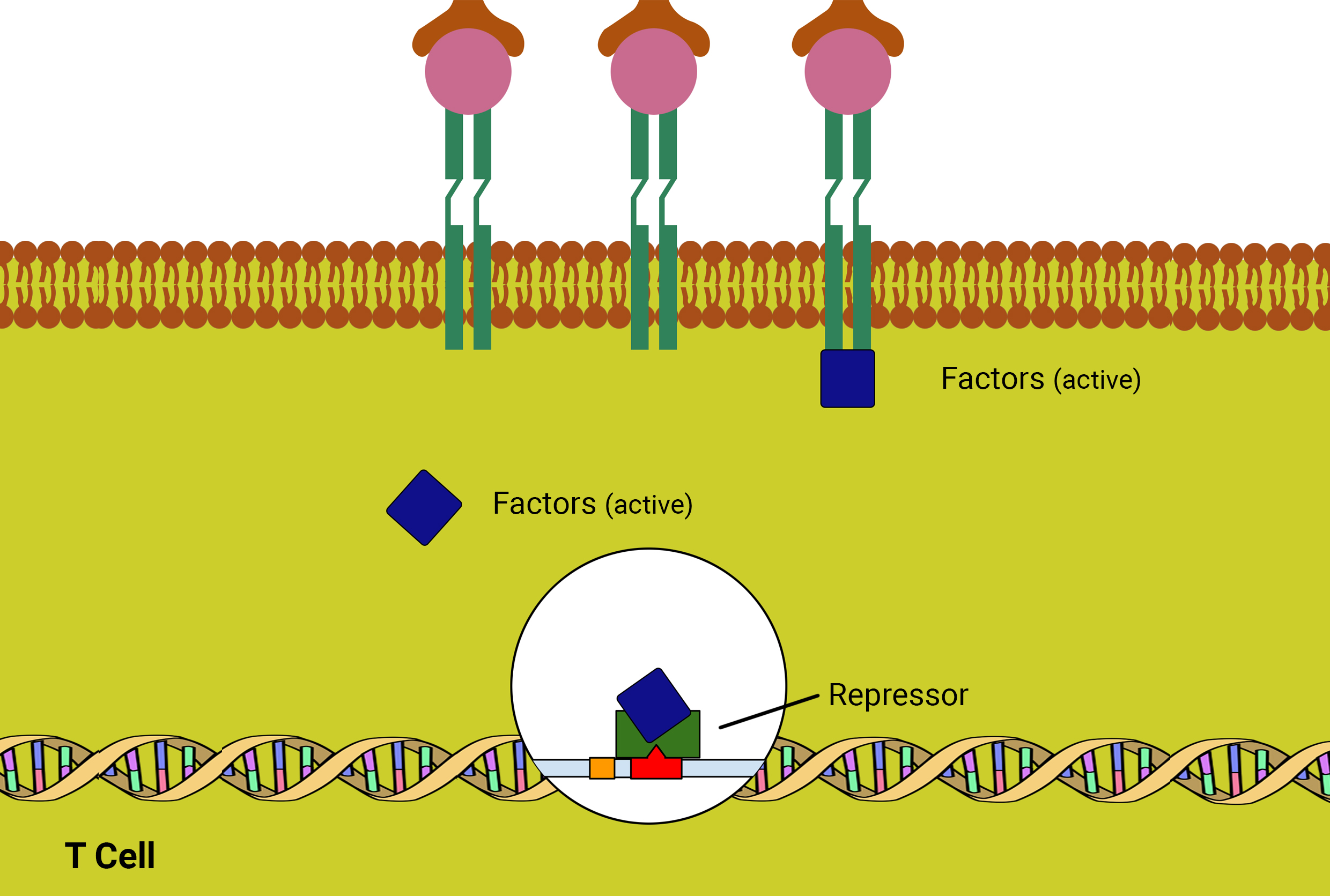
The activated factors are now able to inactivate the repressor allowing RNA Polymerase III to synthesise RNA to create other proteins. This causes the t-cell to create a protein which has a tail sticking off a protease, a transmembrane protein whose extracellular part has a bit of amino acids a tail of venetoclax (Figure 04).
And a protein which can bind to itself, the venetoclax protein, protease protein and the receptor. The attaching protein binds to the receptors (Figure 05).
The vesicles containing the Trans membrane protein head to some of the receptors’ intracellular domain. There they bind to the attaching protein and the protease proteins also bind to the remaining receptors. At last the attaching proteins want to bind to themselves.

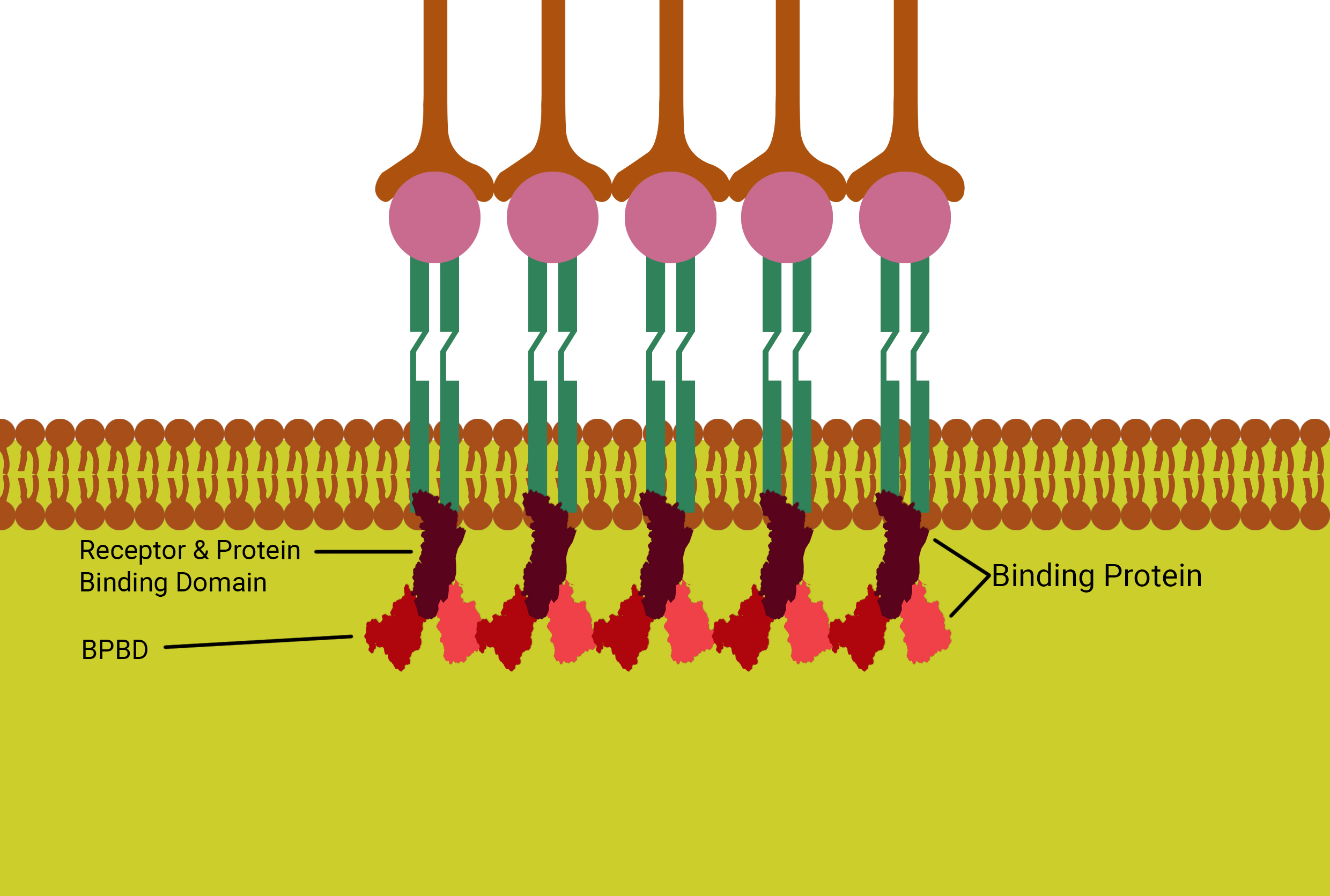
Budding off
The attaching proteins group together and bind to themselves. As because they want to get close, the plasma membrane bends and a sort of ”Virus” buds which is still bound to the Cancer cell.
Maturation
The virus is immature. So, the protease domain cleaves the Venetoclax protein causing the venetoclax part to get separated which causes the virus to get matured. Now, the virus gains its capability to kill the cancer cell.
Entry
Because the receptors are moving the 'virus' gets closer to the cancer cell and fusion occurs. The venetoclax protein then triggers the apoptotic pathway leading to cell death (Figure 06).

- The objective of this receptor is to convert T cell or Blood Vessel Cell into a Cancer Fighting Cell.
Methodology
The Cancer Fighting Cell (Blood Vessel Cell or T cell), is actually a normal cell which is infected by the Lentiviral vector. The cell does not know how to kill the Cancer Cell. Therefore, we need to inject a DNA code that will make the cell to kill the Cancer cell. The DNA that we want to inject is as follows:-
Promoter-Receptor-Factors-repressor-Promoter2-operator-venetoclax-protease-binding_protein
When the Lentivirus injects the DNA, the cell’s machinery makes the proteins encoded in the injected gene. But it can only synthesise the receptor, factors and the repressor because the repressor binds to the operator and further synthesis is blocked. But when the receptors find the antigen present in the Cancer Cell they get activated and then they activate the factors which now are in the active state can bind to the repressor which causes a conformational change in the repressor so that it can’t bind to the DNA anymore causing RNA polymerase III to overcome the barrier formed by the repressor and potentially leading to the synthesis of the Trans membrane Venetoclax Protein, the Protease Protein and the protein which binds all of these are synthesised.
Now the binding proteins bind to the receptors and the remaining proteins bind to the binding proteins. Then the binding proteins want to bind to themselves causing the Plasma membrane to bend and get pinched of creating a sort of “virus”. As the Trans membrane proteins move throughout the cell membrane and they are bound to each other in different membranes their movement causes the virus to get closer. Meanwhile, the protease protein cleaves of a part of the Venetoclax Trans membrane Protein causing the venetoclax part to get separated from its Trans membrane Protein.
After that, due to the close proximity of the virus and the Cancer Cell the two membranes fuse and the Venetoclax Protein gets injected into the Cancer Cell triggering the apoptotic pathway, killing the Cancer Cell. Therefore, the Cancer Fighting Cell wasn’t aware that it killed a Cancer Cell.
Expected Results and Discussion
As a result, it will kill the Cancer cell and unlike the CAR T CELL Therapy it does not destroy the T Cells’ receptor.
As because CAR T CELL Therapy firstly takes in many White Blood Cells (WBC) and secondly destroys their receptors and finally inserts their own receptors. After that the cancer dies out. The receptor may not be recovered because the person may not be infected with the virus so that he/she has copies of that cell or all of the cells are taken and they activate the T cell. While in this project new receptor is introduced and the T cells’ own receptors are preserved. And also the T cell isn’t aware that it killed the Cancer Cell.
*****This project is in its early stage. So, it needs an experimental support & proper guidance by a Professor. *****
Conclusion
In conclusion, this receptor represents a revolution in the field of cancer treatment. By harnessing the power of the immune system and genetically modifying the patient's own T cells, the receptor enhances the ability of these cells to recognize and eliminate cancer cells with high precision.
As it is in its early stage it has to be proven. If it wills success then it will turn into a revolutionized cancer treatment.
© Emon's Lab 2023. All Rights Reserved. Designed by HTML Codex
